Myiasis refers to an infection caused by the infestation of fly larvae (maggot) in human body tissues. These maggots survive by feeding on live or dead host body tissue, body fluids, or ingested food. Myiasis is more commonly observed in tropical regions due to their warmer and humid climates, which provide an ideal environment for fly reproduction.1,2
Maggot infestation is usually found in wild and domestic animals, often due to the smell from their body discharge and poor hygienic living conditions. Such infestations rarely occur in humans.2 Although myiasis can be asymptomatic, it can sometimes lead to serious consequences if maggots invade vital organs, triggering severe sepsis.3 Therefore, it is crucial to raise awareness among the public and for healthcare providers to be vigilant in early detection of myiasis to avoid potential complications in patients. This report presents a case of myiasis in a tracheostomy wound.
Case Report
A 47-year-old gentleman presented to the emergency department with a complaint of bleeding and foul-smelling yellowish discharge from his tracheostomy wound, which had been persisting for three weeks. The patient had been experiencing a crawling sensation in his neck along with localized pain for the past week. The tracheostomy had been performed four months ago due to prolonged ventilation following a severe brain injury sustained in a motor vehicle accident. After his discharge from the hospital, he had been under the care of a private nursing care center.
Upon examination of his neck, it was noted that his tracheostomy tube was entirely blocked by thick crusting, as evidenced by the absence of airflow and confirmed by a bedside flexible fiber-optic endoscope. However, the patient appeared comfortable while breathing room air and was able to speak in full sentence without any signs of respiratory distress or sepsis. Upon lifting the flange of the tracheostomy tube, it was noticed that the surrounding tracheostomy wound was infested with maggots, which were crawling around and burrowing under the subcutaneous tissue [Figure 1]. A bedside nasopharyngolaryngoscopy was performed and confirmed that the patient’s bilateral vocal folds were mobile with evidence of good airway patency. To obtain better wound exposure and visualize the maggots [Figure 2], the blocked tracheostomy tube was decannulated. An attempt was made to remove the maggots from the tracheostomy wound using forceps, but only 35 maggots were removed as the patient could not tolerate the pain despite receiving adequate analgesia. Subsequently, the patient was scheduled for wound exploration and maggot removal under general anesthesia. Meanwhile, a cotton ball soaked with turpentine was packed over the tracheostomy wound to suffocate the remaining maggots while awaiting transfer to the operating theatre. He was started on intravenous cefoperazone 1 g twice daily.
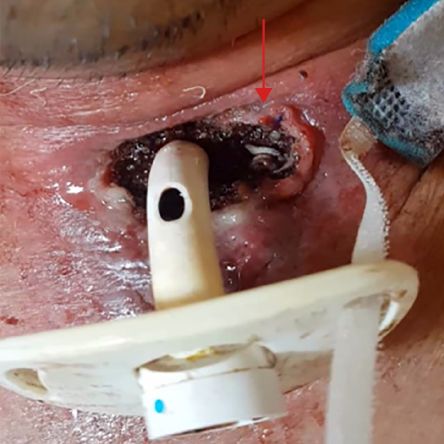 Figure 1: Arrow showing maggots around the tracheostomy wound upon lifting the “Shirley” double lumen tracheostomy tube (size 4; inner diameter 5.0 mm and outer diameter 9.4 mm). The tracheostomy tube was removed for better wound exposure and maggot localization. There was no evidence of maggots hiding inside the tracheostomy tube and the fenestrated window.
Figure 1: Arrow showing maggots around the tracheostomy wound upon lifting the “Shirley” double lumen tracheostomy tube (size 4; inner diameter 5.0 mm and outer diameter 9.4 mm). The tracheostomy tube was removed for better wound exposure and maggot localization. There was no evidence of maggots hiding inside the tracheostomy tube and the fenestrated window.
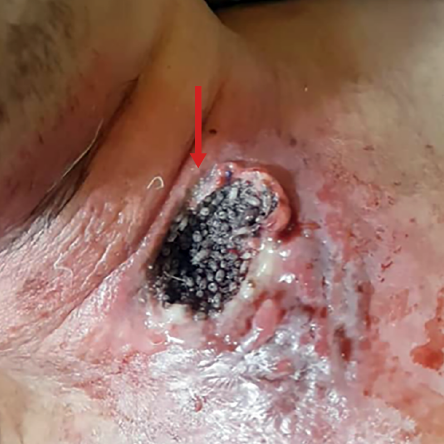 Figure 2: Arrow indicates the maggots fully occupying the entire tracheostomy wound after the tracheostomy tube was decannulated. It should be noted that the skin surrounding the wound appeared erythematous due to the tissue’s inflammatory reaction caused by the maggot infestation.
Figure 2: Arrow indicates the maggots fully occupying the entire tracheostomy wound after the tracheostomy tube was decannulated. It should be noted that the skin surrounding the wound appeared erythematous due to the tissue’s inflammatory reaction caused by the maggot infestation.
In the operating theatre, the patient underwent preoxygenation and received intravenous fentanyl 100 mcg, intravenous propofol 150 mg, and intravenous suxamethonium 100 mg before intubation using a polyvinylchloride endotracheal tube size 7.5 mm. Anesthesia was maintained using sevoflurane as the volatile anesthetic agent, with a minimum alveolar concentration of 1.0 throughout the surgery. During the 40-minute procedure, another 40 maggots were found and removed from the subcutaneous layer surrounding the tracheostomy wound. The necrotic tissue and slough covering the wound were debrided until a clean wound base was achieved. Thorough exploration and inspection of the wound were conducted, extending from the level of the hyoid bone to the suprasternal notch, to ensure no maggots were left behind beyond the strap muscle.
Postoperatively, the patient was monitored in the ward. Despite daily dressing with normal saline, five maggots were found on the tracheostomy wound, which were successfully removed at the bedside using forceps. Daily dressing with normal saline was continued for a week until no further maggots were observed, and the patient was then discharged home with thorough instructions on proper tracheostomy wound care to be carried out by his caregiver.
Informed written consent was obtained from the patient.
Discussion
Although myiasis is a rare occurrence in the human population, it can occur in vulnerable and high-risk groups, especially bedridden patients, those with compromised immune systems, individuals with neglected open wounds, and areas with poor hygiene and proximity to livestock.3,4 In otorhinolaryngology practice, possible natural body cavities for myiasis include the nose (rhinomyiasis), ear (otomyiasis), oral cavity, pharynx, and larynx. Myiasis is most commonly observed in the nose due to its spacious cavity, ease of entry, and relatively less sensitive mucosa compared to the ear.1 While cases of myiasis in tracheostomy wounds are rare, there have been reported cases worldwide.
The management of tracheostomy myiasis can be broadly classified into acute-stage and long-term tracheostomy care.2 In the acute-stage, patients require hospitalization for proper removal of maggots through wound debridement. Close monitoring and administration of broad-spectrum antibiotics are necessary to prevent serious complications such as sepsis. Long-term tracheostomy care is crucial to prevent the recurrence of myiasis, and both the patient and caregiver must be educated on tracheostomy hygiene before discharge. In the case of our patient, although the tracheostomy tube had been decannulated, emphasis was placed on tracheostomy wound care to promote rapid secondary wound healing.
Suffocation of the larvae can be achieved using ether, turpentine, or chloroform to make the maggots exit the host tissue.4 In our reported patient’s case, a cotton ball soaked with turpentine, which was subsequently dried, was used to pack the tracheostomy wound to prevent chemical pneumonitis.
Although myiasis in the tracheostomy wound is usually locally invasive, it can have disastrous consequences if major vessels such as the internal jugular vein or carotid artery are invaded, resulting in massive hemorrhage during the process of mechanical maggot removal.5 Additionally, maggots themselves can serve as a source of emboli, leading to local or distant thrombosis of major blood vessels with potentially fatal outcomes4 Furthermore, there is a risk of maggots migrating into the tracheal lumen, causing airway obstruction and aspiration pneumonitis.6 Fortunately, none of these complications occurred in our patient during his hospitalization and close observation in our otorhinolaryngology ward.
Conclusion
Personal hygiene and proper wound care are essential in preventing myiasis, particularly in tropical countries. Early detection of maggot infestation and prompt treatment by caregivers are crucial in preventing fatal consequences, especially in vulnerable and vegetative individuals.
Disclosure
The authors declared no conflicts of interest.
references
- 1. Arora S, Sharma JK, Pippal SK, Sethi Y, Yadav A. Clinical etiology of myiasis in ENT: a reterograde period–interval study. Braz J Otorhinolaryngol 2009;75(3):356-361.
- 2. Periasamy C, Mohamad I, Johan KB, Hassan NF. Maggots from tracheostoma. Arch Orofac Sci 2013 Mar;8(1):41-43.
- 3. Singh A, Singh Z. Incidence of myiasis among humans-a review. Parasitol Res 2015 Sep;114(9):3183-3199.
- 4. Kumar SP, Ravikumar A, Somu L, Prabhu PV, Subbaraj RM. Tracheostomal myiasis: a case report and review of the literature. Case Rep Otolaryngol 2011;2011:303510.
- 5. Kaya KH. Tracheostomal myiasis in a female patient. Kulak Burun Boğaz Uygulamaları 2014 Dec;2(3):132-134.
- 6. Franza R, Leo L, Minerva T, Sanapo F. Myiasis of the tracheostomy wound: case report. Acta Otorhinolaryngol Ital 2006 Aug;26(4):222-224.