Chronic suppurative otitis media (CSOM) is defined as chronic inflammation of the middle ear, which is characterized by the presence of a tympanic membrane (TM) perforation, which might cause recurrent ear discharge and hearing impairment.1 CSOM is a common public health problem worldwide and is considered relatively common in developing countries.2 It has a significant impact on the social life of an individual due to persistent otorrhea and hearing disability.
The definitive management for CSOM is tympanoplasty. The aim of this surgery includes the prevention of recurrent ear discharge, improvement in hearing, in addition to the ease in hearing aid usage.3 Type 1 tympanoplasty is the repair of the tympanic membrane without reconstructing the ossicles. Many types of grafts and different surgical approaches have been implemented in the past. The most widely used grafts nowadays are temporalis fascia (TF) graft and cartilage graft.3
Despite the routine nature of this surgery, failures have been reported in the literature, and the success rate shows a wide range.4 There are several influencing factors that are presumed to affect the outcome of tympanoplasty, such as age, gender, size of perforation, surgical approach, and type of graft material used. However, despite the presence of many published studies, their effect on the outcome of the surgery is still considered controversial.2
In our study, we sought to evaluate the anatomical and functional outcome of type 1 tympanoplasty and to assess the various factors that might have influenced the outcome.
Methods
The study was a retrospective study which involved all patients who have undergone type I tympanoplasty in the ear, nose, and throat department in Al Nahdha Hospital, Oman, between January 2010 and December 2020. Ethical approval for this study was obtained from the Committee of Medical Research of the Ministry of Health, Oman.
The demographic data of all patients were collected including age and gender. The preoperative examination was collected including the size and the position of the perforation. All patients had a pure tone audiometry (PTA) pre- and postoperatively. Operative details including surgical approach and type of graft used were also collected.
Patients with cholesteatoma and those who had undergone mastoidectomy, ossiculoplasty, or revision tympanoplasty were excluded from the study, in addition to patients with no follow-up after the surgery.
Patients were followed up at intervals (two weeks, one month, three–six months, and one year). The status of the TM was assessed six months postoperatively, in addition to the PTA. The success rate of the surgery in this study was defined as an intact TM and ≥ 10 dB air-bone gap (ABG) closure, six months postoperatively.
The collected data were tabulated in Epidata and statistical analysis was done using SPSS (IBM Corp. Released 2019. IBM SPSS Statistics for Windows, Version 26.0. Armonk, NY: IBM Corp). A p-value of < 0.05 was considered statistically significant. Pre- and post ABG results were compared using the paired t-test. The association between two categorical variables was assessed using the chi-square test.
Results
The total number of cases included in the study was 345. Out of these, 140 (40.6%) were male, and 205 (59.4%) were female. The age range was 14-70 years and the mean age was 37.6 ± 12.0 years. Figure 1 shows the distribution of cases according to different age groups.
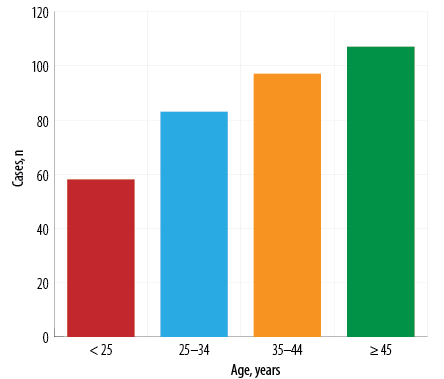 Figure 1: Distribution of cases according to age groups.
Figure 1: Distribution of cases according to age groups.
Most patients (n = 245; 71.0%) had undergone tympanoplasty through the post-aural approach, 59 (17.1%) had the permeatal approach, and the remaining 41 (11.9%) had the endaural approach. A TF graft was used in 236 (68.4%) cases and a cartilage graft in 109 (31.6%) cases [Figures 2 and 3].
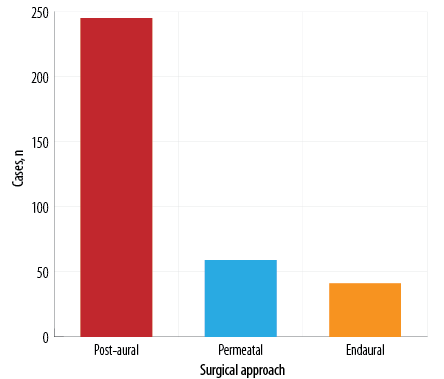 Figure 2: Distribution of cases according to
Figure 2: Distribution of cases according to
surgical approach.
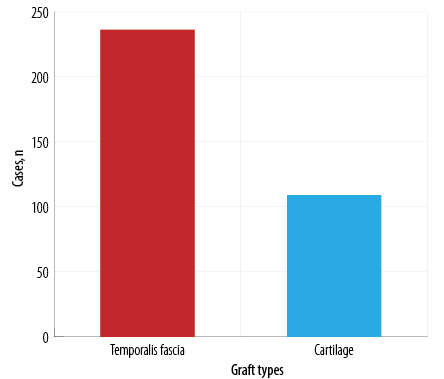 Figure 3: Distribution of cases according to
Figure 3: Distribution of cases according to
graft type.
The follow-up duration was three to six months in 212 (61.4%) cases; six months to one year in 90 (26.1%) cases, and > 1 year in 43 (12.5%) cases.
The graft success rate (intact TM after three to six months) was 84.3% and 54 (15.7%) were found to have a residual perforation [Figure 4]. Out of the 54 cases with residual perforation, 19 (35.2%) required revision surgery.
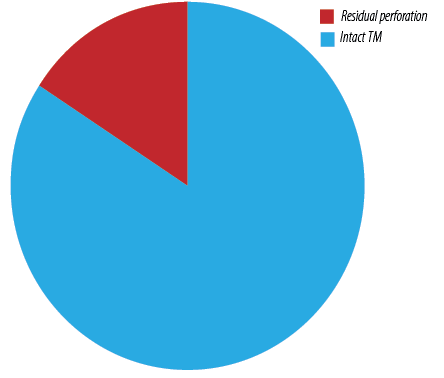 Figure 4: Postoperative tympanic membrane (TM) status at six months.
Figure 4: Postoperative tympanic membrane (TM) status at six months.
The average preoperative air conduction was 38.5 ± 15.3 and the average postoperative air conduction was 25.0 ± 16.1 with a gain of 13.5. The average preoperative ABG was 26.1 ± 9.5 and the average postoperative ABG was 14.4 ± 9.3 with a gain of 11.7. This was statistically significant with a p-value of < 0.001. This is summarized in Table 1. Hearing improvement (≥ 10 dB ABG closure) was seen in 201 (67.0%) patients. Hearing remained the same in 95 patients (31.7%) and worsened in four patients (1.3%) [Table 2].
Table 1: Pre- and postoperative and gain of air conduction and air-bone gap.
|
Air conduction
|
38.5 ± 15.3
|
25.0 ± 16.1
|
13.5
|
< 0.001
|
Table 2: Percentage of hearing improvement.
|
Improved (ABG ≥ 10 dB)
|
201 (67.0)
|
|
Same
|
95 (31.7)
|
ABG: air-bone gap.
Table 3 summarizes the gain in ABG and the graft success rate according to different factors.
Table 3: Graft success rate and gain in air-bone gap (ABG) according to factors.
|
Age, years
|
|
|
|
|
|
< 25
|
17.1
|
0.041
|
44 (75.9)
|
0.273
|
|
25–34
|
13.0
|
|
73 (88.0)
|
|
|
35–44
|
14.0
|
|
82 (84.5)
|
|
|
≥ 45
|
14.2
|
|
92 (86.0)
|
|
|
Sex
|
|
|
|
|
|
Male
|
15.2
|
0.668
|
120 (85.7)
|
0.651
|
|
Female
|
14.8
|
|
171 (83.4)
|
|
|
Perforation size
|
|
|
|
|
|
Small
|
15.1
|
0.644
|
36 (81.8)
|
0.163
|
|
Medium
|
14.6
|
|
131 (88.5)
|
|
|
Large
|
13.6
|
|
103 (83.1)
|
|
|
Subtotal
|
15.2
|
|
21 (72.4)
|
|
|
Surgical approach
|
|
|
|
|
|
Post-aural
|
13.9
|
0.224
|
207 (84.5)
|
0.404
|
|
Permeatal
|
16.0
|
|
52 (88.1)
|
|
|
Endaural
|
14.6
|
|
32 (78.0)
|
|
|
Graft type
|
|
|
|
|
|
Temporalis fascia
|
13.5
|
0.009
|
197 (83.5)
|
0.633
|
The age group of < 25 year had the highest ABG gain of 17.15, p = 0.041, whereas the highest graft success rate was in the 25–34 year group (88.0%), which was not statistically significant. Regarding to gender, the graft success rate in males and female were 85.7% and 83.4%, respectively (p = 0.651). The gain in ABG between males and females was almost the same. Subtotal perforations had the highest gain in ABG of 15.2 dB, and medium-sized perforations had the highest graft success rate of 88.5%, with a p-value of 0.644 and 0.163, respectively. The permeatal approach had the highest gain in ABG of 16.0 dB and the highest graft success rate of 88.1%. Cartilage graft had the highest gain in ABG and graft success rate, with p-values of 0.009 and 0.633, respectively.
Discussion
CSOM is a common disease worldwide, which can be problematic to the patients; recurrent ear discharge is the most common symptom. Tympanoplasty is a common otologic surgery, with a good success rate both anatomically and functionally. In this study, we evaluated the graft success rate and functional outcome in terms of ABG closure after type 1 tympanoplasty in 345 cases.
Regarding the anatomical outcome of our study, the graft success rate was 84.3%. This is comparable to other studies published in the literature. The quoted success rate of type 1 tympanoplasty ranges from 80%–95%.5,6 In a study published by Batni et al,5 the graft success rate was 88%. In another study published by Sajid et al,7 the graft success rate after one year was 80.5%. In a prospective study of 40 cases published by Saha et al,8 the graft success rate was 85%, six months after the surgery. Our study had a similar graft success rate when compared to other studies.
The mean ABG is the most common outcome measure used in tympanoplasty.9 In this study, hearing improvement was measured using gain in ABG pre- and postoperatively. A ABG closure of ≥ 10 dB is considered good hearing improvement. The average preoperative ABG was 26.1 ± 9.5 and the average postoperative ABG was 14.4 ± 9.3, with a gain of 11.7 dB. This was found to be statistically significant with a p-value of < 0.001. The number of patients who had improvement in ABG ≥ 10 dB was 201 (67.0%), the number of patients who had improvement < 10 dB or no change in ABG was 95 (31.7%). Out of these patients, eight had fixed ossicles due to tympanosclerosis. Four patients (1.3%) had worsening of hearing postoperatively, three had fixed ossicles due to tympanosclerosis, and one patient had the hearing test one month after the surgery, which was not repeated.
A study conducted by Thakur et al,4 in 2015 found that 82.8% of patients had improvement in hearing of > 10 dB ABG gain, and 5.3% had worsening of hearing. Aslam et al,6 found that 74% of patients had > 15 dB ABG gain. The rate of hearing improvement in our study is lower than those published in the literature. Most of the studies mentioned had a one-year follow-up period; the majority of our patients were followed up for three to six months. Of the patients who had no improvement in hearing, 61.4% were followed up between three and six months. This could be one reason for having a lower rate of hearing improvement compared to other studies.
Furthermore, this study evaluated a few factors that can influence the outcome. The factors addressed in this study were age, gender, size of perforation, surgical approach, and type of graft used. Age had no influence on the graft success rate; however, we observed a statistically significant better ABG gain in the < 25 years age group. Many authors reported that age does not affect the success of tympanoplasty.3,10 Results of a study conducted by Thakur et al,4 showed that age did not influence the outcome of the surgery. Another study conducted by Mak et al,10 showed that younger age groups had similar results to older age groups. However, Saha et al,8 found that the young age group (< 24 years) had a better postoperative hearing and graft success rate. In our study, gender had no influence on the graft success rate and the gain in ABG. This is consistent with many studies in the literature. Thakur et al,4 reported that the graft success rate in females was 94.6% and 88% in males, which was not statistically significant.
The size of the perforation and surgical approaches were also analyzed as influencing factors and were found to have no effect on the outcome of the surgery in our study. Saha et al,8 evaluated the surgical approach as an influencing factor and reported no difference in the outcome between the post-aural, permeatal, and endaural approaches.
The size of the perforation does not affect the surgical outcome as supported by many studies.4,6 Aslam et al,6 reported that the perforation size had no effect on the graft or hearing improvement success rate. In contrast, Sajid et al,7 reported that smaller-sized perforation had the highest graft success rate and the larger the perforation had the lower success rate.
The use of cartilage graft versus TF graft has always been a controversial subject. Many studies concluded that hearing outcomes in cartilage tympanoplasty are comparable to TF.5 A meta-analysis of 37 studies concluded that the success rate of cartilage graft compared to TF graft was 92% and 82%, respectively, and that hearing outcome was similar in both graft types.11 Similarly, Jain et al,12 reported that graft uptake in TF tympanoplasty was 82.9% and 97.1% in cartilage graft, which was statistically significant. In contrast, Effat reported in his study comparing inlay cartilage with underlay TF, that cartilage had worse graft success (43% vs. 83%).13 We found that the cartilage graft had a statistically significant better ABG closure, and a better, yet not statistically significant, graft success rate when compared to the TF. These results are consistent with other studies.
Other factors evaluated in other studies included the status of the contra-lateral ear and dry or discharging middle ear at the time of surgery. Emir et al,3 reported that the status of the operated ear at the time of the surgery did not influence the success rate. On the other hand, Saha et al,8 found that the graft success rate in patients with bilateral TM perforation was 66%, and 92.8% in those who had a unilateral TM perforation; this was found to be statistically significant. These factors were not included in our study.
One of the limitations of our study is its retrospective nature, which suffers from missing data. Another limitation is that the cases included were done by multiple surgeons, rather than one surgeon. In addition, there were other factors that were not evaluated in this study that could have influenced the outcome of the surgery. Our follow-up duration was three to six months; a longer follow-up might have given a better outcome in terms of hearing improvement. Also, the time interval between the surgery and postoperative PTA varied between the cases.
Conclusion
The graft success rate of type 1 tympanoplasty in Al Nahdha Hospital in the past 10 years was 84.3%, and the ABG closure was 11.7. The percentage of patients who had improvement in ABG closure of ≥ 10dB was 67.0%. These results are comparable with results of other published studies. Factors (age, gender, size of perforation, and surgical approach) that are presumed to influence the outcome of type 1 tympanoplasty were statistically not significant. This is consistent with other studies. Cartilage graft was found to give a better closure of ABG, which was statistically significant. We recommend that further studies be conducted with a longer follow-up period and address more factors to achieve a better insight pertaining to the outcome of type 1 tympanoplasty.
Disclosure
The authors declared no conflicts of interest. No funding was received for this study.
references
- 1. Acuin J. Chronic suppurative otitis media: burden of illness and management.1st ed. Switzerland: World Health Organization, Geneva; 2004. p. 9-10.
- 2. Naderpour M, Moghadam YJ, Ghanbarpour E, Shahidi N. Evaluation of factors affecting the surgical outcome in tympanoplasty. Iran J Otorhinolaryngol 2016 Mar;28(85):99-104.
- 3. Emir H, Ceylan K, Kizilkaya Z, Gocmen H, Uzunkulaoglu H, Samim E. Success is a matter of experience: type 1 tympanoplasty: influencing factors on type 1 tympanoplasty. Eur Arch Otorhinolaryngol 2007 Jun;264(6):595-599.
- 4. Thakur SK, Singh SK, Afaque A, Ghimire N. Outcome of type 1 tympanoplasty: an experience at Biratnagar eye hospital in Eastern Nepal. Asian J Med Sci 2016;7(2):55-60.
- 5. Batni G, Goyal R. Hearing outcome after type I tympanoplasty: a retrospective study. Indian J Otolaryngol Head Neck Surg 2015 Mar;67(1):39-42.
- 6. Aslam N, Iqbal J, Mehmood K. Type I tympanoplasty underlay technique and results. Proc Shaikh Zayed Postgrad Med Inst 2001;15(2):77-80.
- 7. Sajid T, Shah MI, Ghani R, Asif M. Type-I tympanoplasty by underlay technique - factors affecting outcome. J Ayub Med Coll Abbottabad 2017;29(2):258-261.
- 8. Saha AK, Munsi DM, Ghosh SN. Evaluation of improvement of hearing in type I tympanoplasty & its influencing factors. Indian J Otolaryngol Head Neck Surg 2006 Jul;58(3):253-257.
- 9. Matuszewska I, Burduk P, Kaźmierczak W, Janiak-Kiszka J. Functional outcomes of tympanoplasty surgery. Otolaryngol Pol 2016 Nov;70(6):12-19.
- 10. Mak D, MacKendrick A, Bulsara M, Coates H, Lannigan F, Lehmann D, et al. Outcomes of myringoplasty in Australian aboriginal children and factors associated with success: a prospective case series. Clin Otolaryngol Allied Sci 2004 Dec;29(6):606-611.
- 11. Jalali MM, Motasaddi M, Kouhi A, Dabiri S, Soleimani R. Comparison of cartilage with temporalis fascia tympanoplasty: a meta-analysis of comparative studies. Laryngoscope 2017 Sep;127(9):2139-2148.
- 12. Jain A, Samdani S, Sharma MP, Meena V. Island cartilage vs temporalis fascia in type 1 tympanoplasty: a prospective study. Acta Otorrinolaringol Esp (Engl Ed) 2018;69(6):311-317.
- 13. Effat KG. Results of inlay cartilage myringoplasty in terms of closure of central tympanic membrane perforations. J Laryngol Otol 2005 Aug;119(8):611-613.