A seven-year-old boy presented to the pediatric dermatology clinic with a chronic eczematous pruritic eruption that had been present for several months, as well as persistent bilateral lower limb edema. The patient was free of respiratory distress, tachycardia, or mucocutaneous discoloration. His parents denied any history of jaundice, hematuria, or periorbital edema. He maintained a healthy appetite without any reported weight loss, fatigue, or myalgia. He had not traveled to areas with unusual insect exposure or swampy environments. He was born late preterm, with a prenatal diagnosis of hydrops fetalis. Similar symptoms of lower limb edema were observed in his mother and younger brother. Though the parents were not closely related, they shared the same tribal and village background. Focused examination revealed bilateral lower limb edema extending proximally to the mid-thigh with eczematous lesions. The skin displayed scaliness with erosions on the dorsum of both feet [Figure 1]. Informed consent was obtained from the
patient's parents.
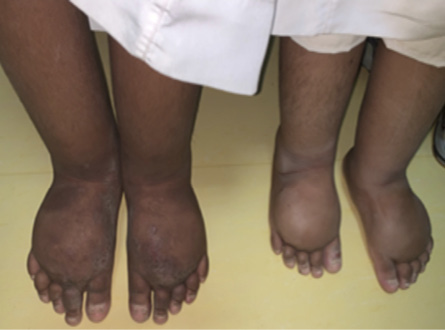 Figure 1: The patient (left) and his sibling, both having bilateral lower limb edema. The patient had an eczematous skin lesion over the dorsum of bilateral feet.
Figure 1: The patient (left) and his sibling, both having bilateral lower limb edema. The patient had an eczematous skin lesion over the dorsum of bilateral feet.
Question
- What is the diagnosis?
a. Congestive heart disease.
b. Cirrhosis.
c. Milroy disease.
d. Malnutrition.
e. Elephantiasis.
Answer
c. Milroy disease.
Discussion
Milroy disease, also known as congenital lymphedema, is an inherited condition with an autosomal dominant pattern.1 It is characterized by underdeveloped or anomalous lymphatic vessels resulting from a mutation in the FLT4 gene, which encodes vascular endothelial growth factor receptor-3. The mutation impedes the normal drainage of lymphatic fluid, leading to protein accumulation in the extracellular fluid. This accumulation stimulates fibroblasts, resulting in swelling and an increased vulnerability to lymphangiomas and recurrent skin infections.2
Lower-limb lymphedema may initially manifest as a pedal-swelling at birth or shortly thereafter, with a potential onset later in life. The severity of the swelling may vary among individuals who carry the same mutation (often within families), typically affecting both legs but with potential asymmetry. Though the edema may continue to progress, temporary remissions may occur, especially in the early years. Additional features associated with Milroy disease include hydrocele (occurring in 37% of males), prominent veins below the knees (in 23% of cases), up-slanting toenails (in 14% of cases), papillomatosis (in 10% of cases), and urethral abnormalities in males (in 4% of cases).1 About 20% of patients, mostly males, may develop cellulitis, which can further harm the lymphatic vessels.1
The diagnosis of Milroy disease relies primarily on molecular genetic testing for a specific FLT4 gene variant. This is crucial for individuals with early-onset lower-limb lymphedema. In our patient, molecular genetic testing detected a variant mutation in exon 19 of the FLT4 gene, c.2735T>G (p.Leu912Arg). Another confirmatory test is lymphoscintigraphy, which reveals a distinctive lack of radioactive colloid absorption in ilioinguinal lymph nodes.1
The treatment strategy for hereditary lymphedema is primarily conservative and involves managing the symptoms and preventing secondary complications. Lower extremities lymphedema is the most frequent medical morbidity seen by dermatologists where the initial mainstay treatment focuses on reducing the edema by wearing pneumatic compressions, stockings, and supportive footwear, along with adjuvant therapies such as weight control, exercise, and massage.1
Prevention of the secondary complications in severe lymphedema such as stasis dermatitis, skin fissuring, and cellulitis involves maintaining good skin hygiene, moisturization, topical corticosteroids, prompt treatment of infections with antibiotics, prophylactic antibiotics for recurrent infections, and active surveillance through regular follow-up in lymphedema-specialized clinics.1
Where conservative treatments are not successful, different surgical approaches can be considered. Microsurgery anastomosis approach involves directly connecting small lymphatic vessels to the venous system. Reduction operation is about the removal of excess fibrous tissue. Recently, vascularized lymph node transfer with therapeutic lipectomy was found to be a reliable technique to open an alternative pathway for lymph drainage to reduce the load on the lymph node. In contrast, therapeutic lipectomy removes excess subcutaneous adipose tissue.3,4
Disclosure
The authors declared no conflicts of interest.
references
- 1. Van Zanten M, Mansour S, Ostergaard P, Mortimer P, Gordon K. Milroy disease. 2006 Apr 27 [Updated 2021 Feb 18]. In: Adam MP, Feldman J, Mirzaa GM, Pagon RA, Wallace SE, Bean LJH, et al, editors. GeneReviews®. Seattle (WA): University of Washington, Seattle; 1993-2023.
- 2. Brice G, Child AH, Evans A, Bell R, Mansour S, Burnand K, et al. Milroy disease and the VEGFR-3 mutation phenotype. J Med Genet 2005 Feb;42(2):98-102.
- 3. Bolletta A, Di Taranto G, Chen SH, Elia R, Amorosi V, Chan JC, et al. Surgical treatment of Milroy disease. J Surg Oncol 2020 Jan;121(1):175-181.
- 4. Park KE, Allam O, Chandler L, Mozzafari MA, Ly C, Lu X, et al. Surgical management of lymphedema: a review of current literature. Gland Surg 2020 Apr;9(2):503-511.